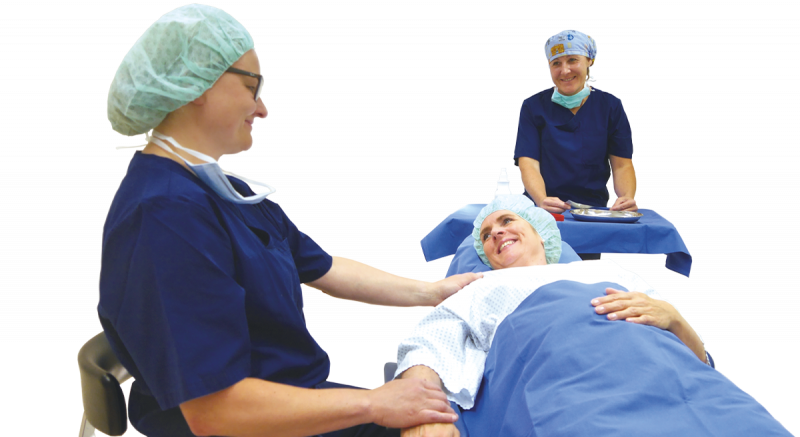
Liposuction
Lipoedema is a disease that causes extreme physical and psychological stress. In order to save patients years of suffering, the available options should be used to correctly diagnose lipoedema and initiate therapy. Weight loss can have a positive effect on the symptoms typical of lipoedema. But it cannot eliminate them.
Due to its effectiveness and long-lasting results, the surgical removal of adipose tissue together with combined physical decongestion therapy (compression therapy, possibly also manual lymph drainage) is an essential part of the treatment of lipoedema.
While the conservative method of combined physical decongestion therapy (manual lymphatic drainage and compression garment) is able to reduce swelling or orthostatic oedemas and improve the tenderness of the tissue, liposuction is used to reduce the fat tissue and regain normal body proportions. Additionally it also improves the symptoms typical of lipoedema enormously. But it can’t eliminate it completely.
However, liposuction can greatly improve the quality of life of a patient so that it is almost possible to lead a symptomless life (Fig. 1).
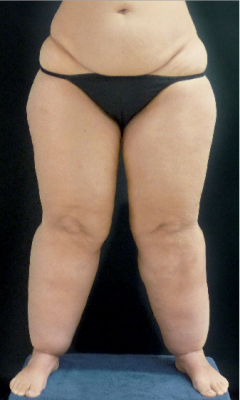
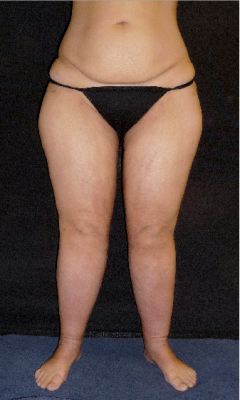 Fig. 1: 39-year-old patient: a. initial situation, b. after liposuction of 9200ml in three sessions
Fig. 1: 39-year-old patient: a. initial situation, b. after liposuction of 9200ml in three sessions
Our technique: local tumescent anesthesia and vibration-assisted liposuction (PAL)
There are a number of different liposuction techniques, such as laser, radio frequency and ultrasound-assisted liposuction.
But since the introduction of tumescent local anesthesia (TLA) and vibration liposuction (PAL) as well as water-jet assisted liposuction (WAL), these techniques have become the first choice methods. Both of them operate with vibrating blunt suction cannulas and make liposuction less risky for the patient and much gentler on the tissue and lymphatic vessels. At the Hanse-Klinik we work with vibration liposuction (PAL: "power assisted liposuction").
Tumescent local anesthesia (TLA) is a form of local anesthesia in which the subcutaneous fatty tissue is filled with large amounts of a diluted anesthetic solution. The Latin word for swelling “tumescere” refers to the plump appearance of the region filled with solution, which is typical for the method.
Before the operation, the involved areas are marked and photographed (Fig. 2). General anesthesia is not required for liposuction.
The infiltration phase lasts about 45 minutes, followed by a 30-minute break. The duration of the suction process itself is averagely between 90 and 150 minutes, depending on the size of the area.
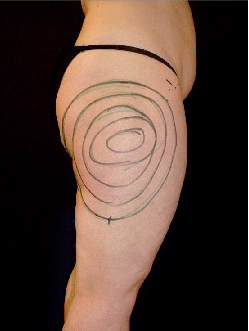
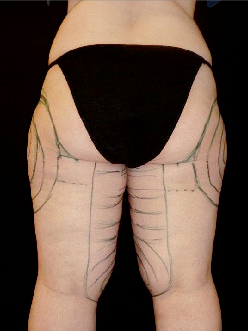
Fig. 2: Preoperative marked suction areas
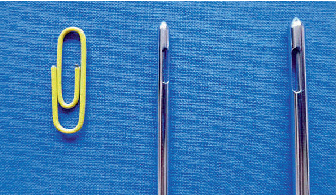
Abb. 3: Blunt suction cannulas
The subsequently achieved high tissue pressure causes the fatty tissue to loosen. Thanks to this “plasticizer effect”, thin (3-4 mm) and at the front blunt suction probes (Fig.3) with small openings on the side can be used. With vibration liposuction, the vibrating suction probe slides past the connective tissue structures without sucking them into the cannula. This significantly reduces the shearing forces and ensures that the fatty tissue that has been “loosened” by the tumescent local anesthetic solution can reach the cannulas more easily. This enables a largely gentle procedure in which the connective tissue support structure of the subcutaneous fatty tissue is preserved.
The edges of the wounds are not sewn, but rather covered with a liquid-permeable plaster. In the first few hours directly after the operation most of the tumescent local anesthesia remaining in the tissue, flows through the skin incisions and is absorbed by the bandages under the compression garment. The remaining amount of fluid drains off within the next 2-5 days. The compression garment must be worn for at least another 8 weeks after the operation. Furthermore, the postoperative manual lymph drainage supports the drainage and reduces the tendency to swell.
The main reason to use this method for liposuction in lipoedema is that it is particularly gentle on the lymphatic vessels and thus the lymphatic drainage continues to be guaranteed after the operation. In addition, the organism is not additionally stressed by general anesthesia. The patient can stand up again immediately after the operation so that the result can be assessed while standing. Not only will the tumescent solution begin to flow through the lowest located incision, but the surgeon can assess the new body silhouette and make corrections if necessary. Already the next morning you can see a clear difference to the initial condition (Fig. 4).
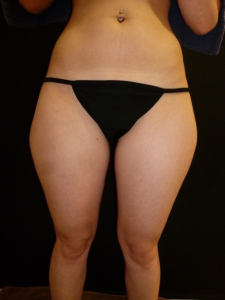
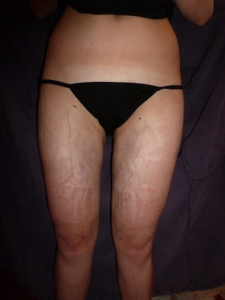
Abb. 4: 29-year-old female patient the next morning after liposuction of the outer thighs, the inner thighs and the inner knees
This method offers many advantages. Due to the very small incisions, there is little intraoperative bleeding and few postoperative hematomas. Due to the wash-out effect of the TLA solution, hardly any bacteria can enter and the risk of infection is very reduced. The antithrombotic effect of the TLA and the immediate postoperative mobilization the risk of thrombosis is greatly reduced. In summary, it can be said that the general complication rate is very low with this method.



